Summary
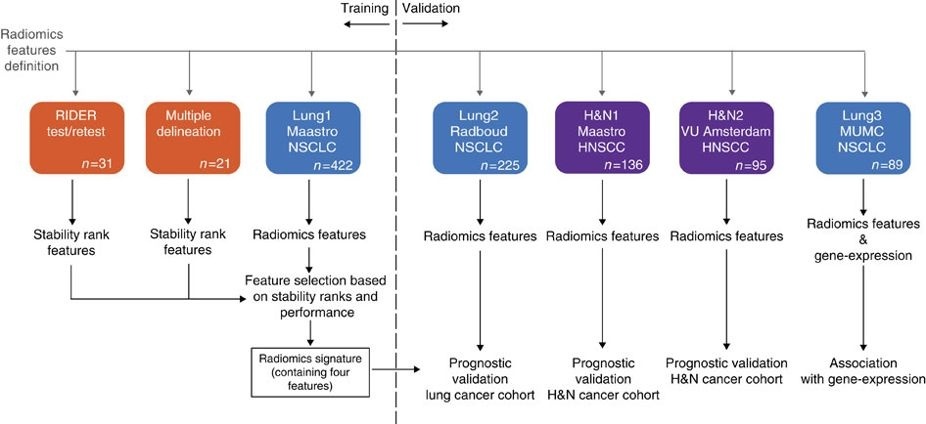
In short, this publication applies a radiomic approach to computed tomography data of 1,019 patients with lung or head-and-neck cancer. Radiomics refers to the comprehensive quantification of tumour phenotypes by applying a large number of quantitative image features. In present analysis 440 features quantifying tumour image intensity, shape and texture, were extracted. We found that a large number of radiomic features have prognostic power in independent data sets, many of which were not identified as significant before. Radiogenomics analysis revealed that a prognostic radiomic signature, capturing intra-tumour heterogeneity, was associated with underlying gene-expression patterns. These data suggest that radiomics identifies a general prognostic phenotype existing in both lung and head-and-neck cancer. This may have a clinical impact as imaging is routinely used in clinical practice, providing an unprecedented opportunity to improve decision-support in cancer treatment at low cost. The DICOM Radiotherapy Structure Sets (RTSTRUCT) and DICOM Segmentation (SEG) files in this data contain a manual delineation by a radiation oncologist of the 3D volume of the primary gross tumor volume ("GTV-1") and selected anatomical structures (i.e., lung, heart and esophagus). Of note, DICOM SEG objects contain a subset of annotations available in RTSTRUCT.
The dataset described here (Lung1) was used to build a prognostic radiomic signature. The Lung3 dataset used to investigate the association of radiomic imaging features with gene-expression profiles consisting of 89 NSCLC CT scans with outcome data can be found here: NSCLC-Radiomics-Genomics.
Other data sets in the Cancer Imaging Archive that were used in the same study published in Nature Communications: Head-Neck-Radiomics-HN1, NSCLC-Radiomics-Interobserver1, RIDER Lung CT Segmentation Labels from: Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach.
For scientific inquiries about this dataset, please contact Dr Leonard Wee (leonard.wee@maastro.nl) and Prof Andre Dekker (andre.dekker@maastro.nl) at MAASTRO Clinic/Maastricht University Medical Centre+ and Maastricht University, The Netherlands.
Acknowledgements
We would like to acknowledge the individuals and institutions that have provided data for this collection:
- Leonard Wee, MAASTRO (Dept of Radiotherapy), Maastricht University Medical Centre+, Maastricht, Limburg, The Netherlands.
- Dirk de Ruysscher, MAASTRO (Dept of Radiotherapy), Maastricht University Medical Centre+, Maastricht, Limburg, The Netherlands.
- Andre Dekker, MAASTRO (Dept of Radiotherapy), Maastricht University Medical Centre+, Maastricht, Limburg, The Netherlands.
- Hugo Aerts, Computational Imaging and Bioinformatic Laboratory, Dana-Farber Cancer Institute & Harvard Medical School, Boston, Massachusetts, USA.
- Harmonization of the components of this dataset, including into standard DICOM representation, was supported in part by the NCI Imaging Data Commons consortium. NCI Imaging Data Commons consortium is supported by the contract number 19X037Q from Leidos Biomedical Research under Task Order HHSN26100071 from NCI.
Data Access
Click the Download button to save a ".tcia" manifest file to your computer, which you must open with the NBIA Data Retriever. Click the Search button to open our Data Portal, where you can browse the data collection and/or download a subset of its contents.
| Data Type | Download all or Query/Filter |
|---|---|
| Images, Segmentations, and Radiation Therapy Structures (DICOM, 33GB) | (Requires the NBIA Data Retriever.) |
| Lung1 clinical (CSV) |
Click the Versions tab for more info about data releases.
Third Party Analyses of this Dataset
TCIA encourages the community to publish your analyses of our datasets. Below is a list of such third party analyses published using this Collection:
Detailed Description
Collection Statistics | |
|---|---|
Modalities | CT, RTSTRUCT, SEG |
Number of Participants | 422 |
Number of Studies | 422 |
Number of Series | 1265 |
Number of Images | 52073 |
| Image Size (GB) | 33 |
Radiation Oncologist Tumor Segmentations
The DICOM Radiotherapy Structure Sets (RTSTRUCT) and DICOM Segmentation (SEG) files in this data contain a manual delineation by a radiation oncologist of the 3D volume of the primary gross tumor volume ("GTV-1") and selected anatomical structures (i.e., lung, heart and esophagus). Of note, DICOM SEG objects contain a subset of annotations available in RTSTRUCT.
For viewing the annotations the authors recommend 3D Slicer that can be used to view both RTSTRUCT and SEG annotations (make sure you install the SlicerRT and QuantitativeReporting extensions first!). Visualization of the DICOM annotations is also supported by the OHIF Viewer.
Other tools include:
- Dicompyler is an open source, cross-platform DICOM RT viewer.
- The Radiotherapy DICOM toolkit, which may also be useful for working with this data.
- dcmqi and Plastimatch libraries can be used to support conversion of the DICOM SEG and RTSTRUCT representations, respectively, into the popular research formats, such as NIfTI or NRRD.
Clinical Data
Corresponding clinical data can be found here: Lung1.clinical.csv.
Please note that survival time is measured in days from start of treatment. DICOM patients names are identical in TCIA and clinical data file.
Citations & Data Usage Policy
Users of this data must abide by the Creative Commons Attribution-NonCommercial 3.0 Unported License under which it has been published. Attribution should include references to the following citations:
Data Citation
Aerts, H. J. W. L., Wee, L., Rios Velazquez, E., Leijenaar, R. T. H., Parmar, C., Grossmann, P., … Lambin, P. (2019). Data From NSCLC-Radiomics [Data set]. The Cancer Imaging Archive. https://doi.org/10.7937/K9/TCIA.2015.PF0M9REI
Publication Citation
Aerts, H. J. W. L., Velazquez, E. R., Leijenaar, R. T. H., Parmar, C., Grossmann, P., Cavalho, S., … Lambin, P. (2014, June 3). Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach. Nature Communications. Nature Publishing Group. http://doi.org/10.1038/ncomms5006 (link)
TCIA Citation
Clark K, Vendt B, Smith K, Freymann J, Kirby J, Koppel P, Moore S, Phillips S, Maffitt D, Pringle M, Tarbox L, Prior F. The Cancer Imaging Archive (TCIA): Maintaining and Operating a Public Information Repository, Journal of Digital Imaging, Volume 26, Number 6, December, 2013, pp 1045-1057. (paper)
Questions may be directed to help@cancerimagingarchive.net.
Other Publications Using This Data
TCIA maintains a list of publications that leverage our data. If you have a publication you'd like to add, please contact the TCIA Helpdesk.
Version 4 (Current): Updated 2020/10/22
| Data Type | Download all or Query/Filter |
|---|---|
| Images (DICOM, 33 GB) | (Requires the NBIA Data Retriever.) |
| Lung1 clinical (CSV) |
- RTSTRUCT and SEG study instance UID changed to match study instance uid with associated CT image.
- Added missing structures in SEG files to match associated RTSTRUCTs.
- Patient Id copied to Patient Name in CT images (for consistency).
- Added 1 missing image for LUNG1-246.
Version 3: Updated 2019/10/23
| Data Type | Download all or Query/Filter |
|---|---|
| Images (DICOM, 29GB) | (Requires the NBIA Data Retriever.) |
| Lung1 clinical (CSV) |
- Re-checked and updated the RTSTRUCT files to amend issues in the previous submission due to missing RTSTRUCTS or regions of interest that were not vertically aligned with the patient image.
- In 4 cases (LUNG1-083,LUNG1-095,LUNG1-137,LUNG1-246) re-submitted the correct CT images.
- The regions of interest now include the primary lung tumor labelled as “GTV-1”, as well as organs at risk.
- For one case (LUNG1-128) the subject does not have GTV-1 because it was actually a post-operative case; we retained the CT scan here for completeness.
- Added DICOM SEGMENTATION objects to the collection, which makes it easier to search and retrieve the GTV-1 binary mask for re-use in quantitative imaging research.
- Clinical data updated as follow-up time has been extended.
Version 2: Updated 2016/05/31 (version 2 removed as RTSTRUCTs or regions of interest were not vertically aligned with patient images. See version 3 for updated files).
| Data Type | Download all or Query/Filter |
|---|---|
| Images (DICOM, 25GB) | not available, see version 3 |
| Lung1 clinical (CSV) |
Added 318 RTSTRUCT files for existing subject imaging data
Version 1: Updated 2014/07/02
| Data Type | Download all or Query/Filter |
|---|---|
| Images (DICOM, 25GB) | the NBIA Data Retriever. |
| Lung1 clinical (CSV) |